Gastric and Duodenal Ulcers: Causes, Symptoms, and Treatment Options
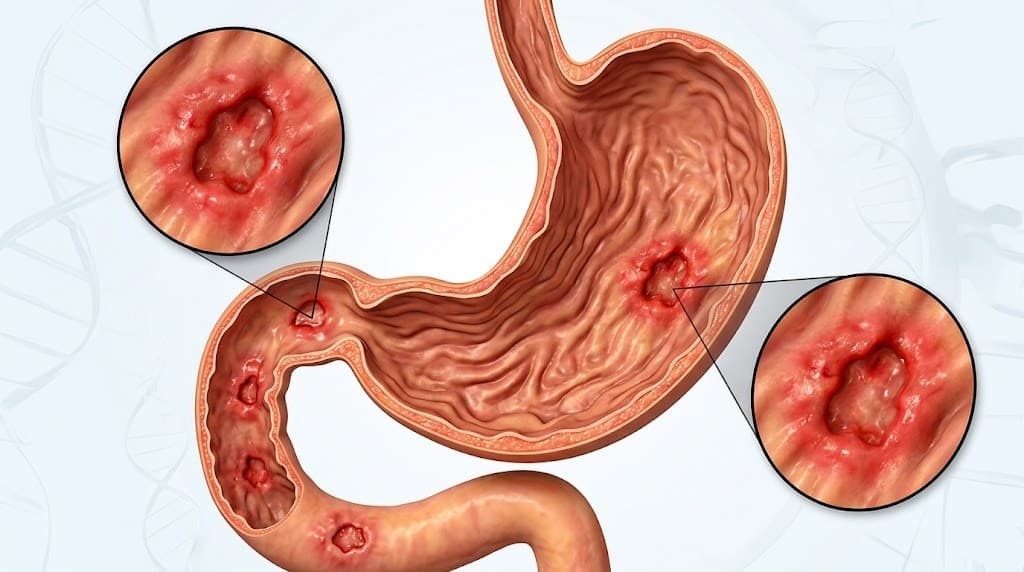
Stomach and duodenal (duodenum) ulcers are tissue losses that occur on the inner surface of these organs due to the effects of stomach acid and digestive enzymes. This condition can progress deeper into the tissue under the influence of acid and digestive fluids, causing wounds and inflammation. Ulcers are a digestive system disease that is common worldwide and can lead to serious health problems.
What Are the Causes of Ulcers?
The most common cause of stomach and duodenal ulcers is a bacterial infection called Helicobacter pylori. Another important factor is the regular use of non-steroidal anti-inflammatory drugs (NSAIDs), especially aspirin and various rheumatism medications, over a long period. Other risks such as genetic predisposition, chronic stress, corticosteroid-like drugs, smoking, alcohol consumption, excessive caffeine intake (for example, coffee), and environmental factors can also contribute to the development of ulcers. However, the effect of these factors may vary from person to person.
At What Ages and In Whom Are Ulcers Most Common?
Although ulcers can develop at any age, duodenal ulcers are most frequently seen between the ages of 30 and 50 and are more common in men. In contrast, stomach ulcers become more prevalent at older ages, especially in women over the age of 60. According to various studies, the proportion of individuals diagnosed with ulcers in the community at any given time ranges from 2% to 6%. Duodenal ulcers are more common than stomach ulcers.
What Are the Symptoms of Ulcers?
The main symptom of stomach and duodenal ulcers is usually a burning or gnawing pain felt in the upper abdominal region. This pain typically increases with hunger, may occur between meals or at night, and can be severe enough to wake the patient from sleep. The pain may subside after eating or taking antacid medications. Less commonly, individuals with ulcers may also experience complaints such as nausea, vomiting, loss of appetite, and involuntary weight loss. Especially, the reduction of pain after vomiting is typical for ulcers. In some periods (for example, in spring and autumn), complaints may increase.
What Are the Serious Consequences of Ulcers?
Bleeding: Ulcers are the most common cause of upper digestive system bleeding. Sometimes, bleeding may be the first sign in people who have not previously been diagnosed with an ulcer. Passing dark brown or black (tarry) stools or vomiting "coffee ground"-like material is considered an important warning sign. Sudden weakness and cold sweating may also indicate bleeding. If these symptoms are observed, it is necessary to seek medical attention without delay.
Perforation (Rupture): If the ulcer deepens and completely penetrates the wall of the stomach or duodenum, stomach acid and digestive enzymes leak into the abdominal cavity, causing sudden and severe abdominal pain. The abdominal muscles become rigid and the person has difficulty moving. This is a life-threatening condition that requires emergency surgical intervention.
Obstruction: Especially in the pyloric region located at the exit of the duodenum or stomach, severe ulcer, tissue swelling, or long-term scar development may result in narrowing and even obstruction. In this case, food and liquids cannot leave the stomach, and the patient vomits frequently and in large amounts. Malnutrition and rapid weight loss may develop. In such cases, rapid diagnosis and surgical intervention may be required.
Which Methods Are Used to Diagnose Ulcers?
A detailed medical history and physical examination are important for diagnosing patients suspected of having an ulcer. However, physical examination or ultrasound generally does not provide specific findings for ulcers. In practice, it is often recommended to try medications that reduce stomach acid and observe whether complaints improve. A definitive diagnosis is made by upper digestive system endoscopy (esophagogastroduodenoscopy). During endoscopy, the esophagus, stomach, and duodenum are directly visualized, and if necessary, biopsies can be taken from suspicious areas. Although barium stomach-duodenum radiography can also be performed, endoscopy is more commonly preferred today.
Which Methods Are Effective in the Treatment of Ulcers?
Drug Therapy:
The main option in modern treatment is medications that reduce stomach acid production, such as proton pump inhibitors (omeprazole, lansoprazole, etc.) and H2 receptor blockers (ranitidine, famotidine, nizatidine, etc.). These drugs support the healing of the ulcer and relieve symptoms. If Helicobacter pylori infection is detected, eradicating this bacterium with appropriate antibiotics is also an important part of treatment. The duration and combination of treatment may vary depending on the location, size of the ulcer, and the patient's overall health status.
Surgical Intervention:
Many ulcers heal successfully with drug therapy. However, if complications such as bleeding, perforation, or obstruction develop, or if the ulcer does not improve despite drug therapy, surgical intervention may be required.
Nutrition and Lifestyle:
In the past, a strict diet was recommended for patients with ulcers; however, it is now known that a special diet does not directly contribute to ulcer healing. It is generally sufficient for the person to pay attention to which foods increase their complaints and to limit them. In addition, since smoking delays the healing of ulcers, quitting is recommended. Avoiding alcohol intake and unnecessary medication use (especially aspirin and NSAIDs) is also important in the treatment of ulcers.
Reducing stress factors, regular and healthy nutrition, and adequate sleep are general health measures that also positively contribute to the healing process of ulcers.
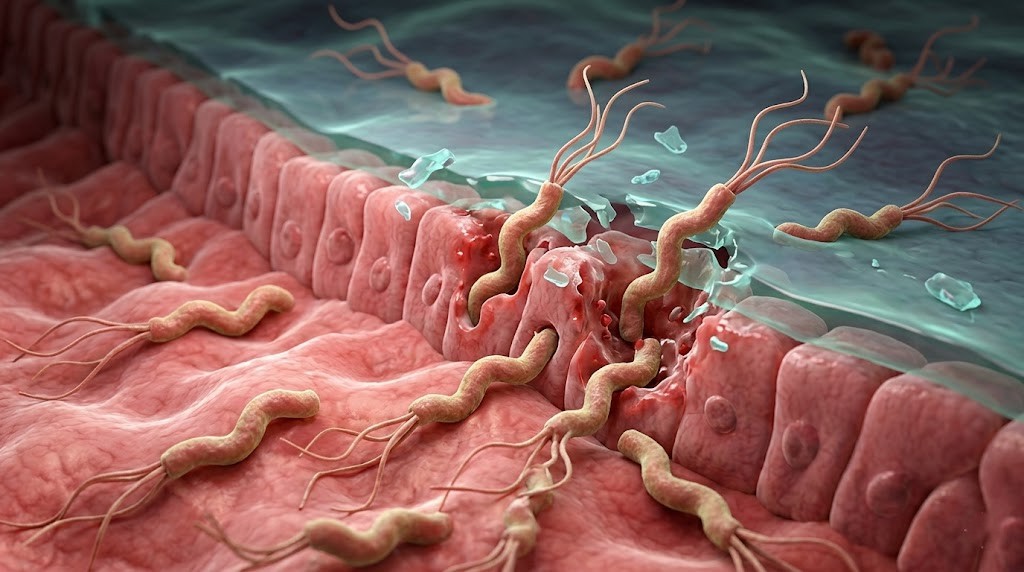
Relationship Between Helicobacter pylori and Ulcers
Helicobacter pylori is the main cause of many ulcer cases. The prevalence of this bacterium is quite high in duodenal ulcers. However, in some people, even though this bacterium is present, ulcers may not develop; therefore, it is thought that other genetic and environmental factors also play a role. Helicobacter pylori can also cause chronic gastritis in addition to ulcers, and some studies show that this bacterium may slightly increase the risk of stomach cancer.
Frequently Asked Questions
1. Can an ulcer heal completely?
Most ulcers can heal completely with proper drug therapy and, if there is a bacterial infection, with appropriate antibiotics. However, it is important to remain vigilant against the risk of recurrence.
2. How is Helicobacter pylori transmitted?
This bacterium can usually be transmitted easily from person to person, orally or in environments with poor hygiene conditions.
3. What should be considered to prevent ulcer recurrence?
Even after treatment is completed, smoking, unnecessary painkillers, and alcohol consumption should be avoided; healthy nutrition and hygiene rules should be followed.
4. What is the role of diet in ulcer treatment?
Although a special ulcer diet is not recommended, the main advice is to avoid foods that cause discomfort to the individual.
5. Does ulcer bleeding pose a life threat?
Severe bleeding can be life-threatening. In case of symptoms such as black stools or brown vomiting, a doctor should be consulted urgently.
6. Which medications trigger ulcers?
Aspirin, ibuprofen, and other NSAID-type painkillers increase the risk of ulcers when used for a long time.
7. Does stress cause ulcers?
Stress alone is not a cause of ulcers; however, it can facilitate ulcer formation by increasing stomach acid or weakening the immune system.
8. What is the most prominent symptom of an ulcer?
It is usually a burning or gnawing pain in the upper abdomen, especially when hungry.
9. Is Helicobacter pylori always treated when detected?
Treatment is recommended in patients with active ulcers or findings of chronic gastritis.
10. Can children get ulcers?
Yes, although rare, ulcers can also be seen in children. If symptoms are present, a pediatric gastroenterology specialist should be consulted.
Endoscopy is generally a short, well-tolerated procedure that can usually be made comfortable with sedative medication.
12. Is lifelong medication necessary after ulcer treatment?
Most patients do not need medication after treatment is completed. However, if risk factors (e.g., NSAID use) persist, long-term treatment may be required according to the physician's recommendation.
References
World Health Organization (WHO) – Peptic Ulcer Disease Factsheet
American College of Gastroenterology – Guidelines on Diagnosis and Management of Peptic Ulcer Disease and H. pylori Infection
Mayo Clinic – Peptic Ulcer Disease
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) – Definition & Facts for Peptic Ulcers
Global Helicobacter pylori Study Group – H. pylori and Gastric Diseases
American Gastroenterological Association – Patient Care Resources on Ulcer Disease