Cervical Disc Herniation: Causes, Symptoms, Diagnosis, and Treatment Processes
What is a Cervical Herniated Disc?
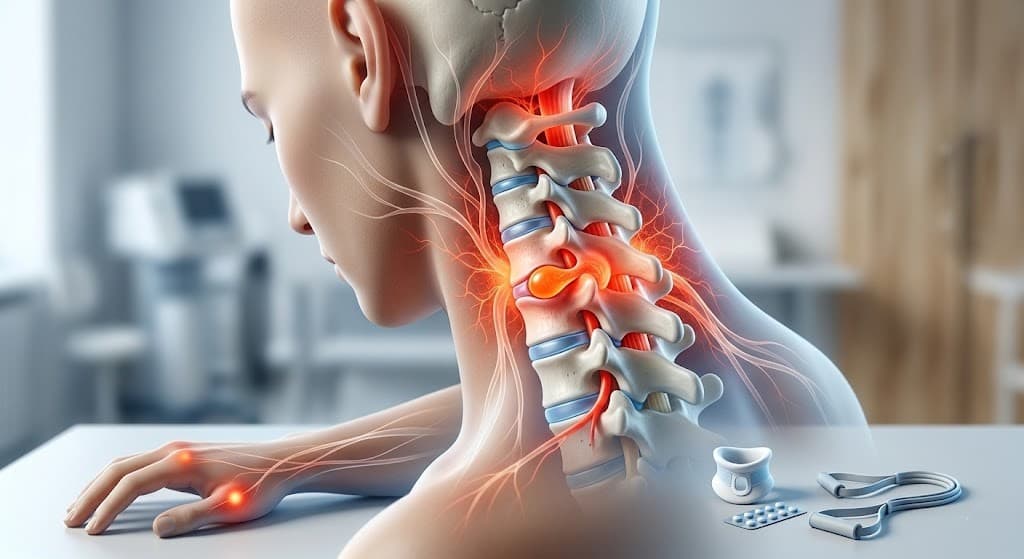
A cervical herniated disc is a health problem that can affect quality of life, occurring when the central part (nucleus pulposus) of the discs located between the vertebrae slips out of place and puts pressure on nearby nerve structures. It is often associated with factors such as heavy lifting, sudden strains, trauma, or prolonged inactivity. Although it can be seen in both young adults and the elderly, it is most commonly encountered between the ages of 20 and 40. In its development, genetic predispositions can be as influential as lifestyle and environmental factors.
How Does a Cervical Herniated Disc Occur?
The spine is one of the main structures that enables the body to stand upright and move. Between the seven vertebrae in the neck region, there are elastic tissues called discs. The soft and gelatinous material (nucleus pulposus) that forms the inner part of the discs is surrounded by a strong ring (anulus fibrosus). When this structure is damaged, the inner material may protrude outward and press on the nerves, causing various complaints.
What are the Causes of Cervical Herniated Disc?
There are often multiple factors involved in the development of a cervical herniated disc. The most common causes include:
Sudden movements, trauma, or impacts
Prolonged inactivity and poor posture habits
Heavy lifting or excessive physical strain
Loss of water and elasticity in the discs due to aging (degeneration)
Smoking
Working for long periods on a computer or with a smartphone
Negative effects of stress on spinal muscles
Family history of similar diseases, that is, genetic predisposition
In addition, cervical herniated disc is more frequently seen in certain occupational groups (for example; those who work at a desk for long periods, those heavily involved in housework, drivers, etc.).
Changes brought by aging can accelerate the deterioration of the natural structure of the disc and pave the way for the development of chronic herniation. In cases of cervical herniated disc that develop suddenly after trauma, complaints usually begin more quickly and distinctly.
What are the Symptoms of Cervical Herniated Disc?
A cervical herniated disc can manifest itself in different ways depending on the severity of symptoms and which nerve root is affected. The most common symptoms are as follows:
Pain in the neck, shoulder, back, and arms
Numbness, tingling, or decreased sensation in the arms or hands
Muscle weakness, especially grip weakness in the arm or fingers
Loss of reflexes or decreased reflex response
General complaints such as headache or dizziness
In rare cases, loss of balance, ringing in the ears, or thinning of the arms
In some individuals, pain may increase with activities such as coughing, sneezing, or straining. The level at which the nerve roots are affected determines in which areas of the arm and hand sensory or motor loss will occur.
In untreated and progressive cases, serious sensory loss or muscle paralysis may develop as a result of nerve compression, so it is important to consult a doctor without delay when symptoms appear.
Symptoms in Nerve Roots Associated with Cervical Herniated Disc
Depending on the level at which the herniation exerts pressure, it may cause various complaints in different nerve roots:
C2: Headache, sensitivity in the eyes and ears
C3, C4: Mild pain and muscle spasm in the neck, shoulder, and back
C5: In addition to neck and shoulder pain, sensory loss and decreased muscle strength in the upper arm and shoulder
C6: Sensory loss and weakness on the lateral side of the shoulder, arm, and hand, decreased wrist reflex
C7: Decreased sensation in the forearms and middle finger, impairment of the triceps reflex
C8-T1: Sensory loss in the hands and the middle part of the forearm, restriction in finger movements
How is Cervical Herniated Disc Diagnosed?
A detailed physical examination is first performed in the diagnosis of cervical herniated disc, and the course of symptoms is carefully evaluated. Especially the spread of pain, onset time, severity, and accompanying neurological findings guide the physician. While laboratory tests are rarely helpful, the main diagnosis is supported by radiological examinations:
X-ray: Visualizes the bony structure of the spine and possible degenerative changes.
Computed Tomography (CT): Used to assess bone details and calcifications in the discs.
Magnetic Resonance Imaging (MRI): Provides the most detailed information about soft tissues, disc herniation, and the degree of nerve root involvement; it is the most sensitive method for diagnosing cervical herniated disc.
Electromyography (EMG) and nerve conduction studies: Can show problems with the electrical conduction capacity of nerves, especially helpful in detecting specific nerve root involvement.
The doctor may also request relevant tests to rule out underlying rheumatic diseases, tumors, or infections.
Approaches Used in the Treatment of Cervical Herniated Disc
The aim of treatment for cervical herniated disc is to alleviate the patient's complaints, reduce nerve compression, and improve quality of life. Treatment is planned individually according to the severity and course of the disease. The first preferred methods are usually non-surgical:
Education and lifestyle recommendations: It is important to establish correct posture and an ergonomic working environment, and to avoid heavy lifting and movements that strain the neck.
Physical therapy and exercise programs: Exercises that strengthen the neck muscles help increase flexibility and blood circulation. However, these exercises must be performed under specialist supervision.
Local heat or cold applications: Can be used to relieve pain and muscle spasm.
Painkillers and muscle relaxants: Used at the prescribed dose and duration.
Spinal injections: In cases of severe pain, corticosteroid injections into the nerve root or epidural area may be applied if deemed appropriate by the physician; this can reduce edema and inflammatory response around the nerve.
Use of a cervical collar: May provide short-term relief in the acute period, but long-term use is not recommended.
Surgical intervention is considered only in severe cases with advanced nerve compression, muscle weakness, or when other treatments fail. In surgery, the part of the disc pressing on the nerve is usually removed. In some special cases, prosthetic disc applications or other surgical procedures to relieve narrowing in the area may be preferred.
In Which Cases is Cervical Herniated Disc Surgery Necessary?
Surgical treatment is not required for all patients with cervical herniated disc. However, surgery may be recommended in the following cases:
Progressive muscle weakness and increasing sensory loss
Pain that does not respond to other treatments and severely restricts daily life
Severe compression of the nerve root and/or risk of paralysis
Impairment of bladder or bowel control
The most appropriate treatment option is determined by evaluating each patient's condition individually.
What Practices are Beneficial for Cervical Herniated Disc?
Various methods can be utilized in the treatment of cervical herniated disc:
Physical therapy and personalized exercises performed under specialist supervision
Muscle relaxants, painkillers, and anti-inflammatory drugs when necessary
Cold or hot compress applications
Massage or chiropractic practices if deemed appropriate by the physician
Choosing a suitable pillow to support neck position and ergonomic lifestyle adjustments
The most important point to remember is to always consult a healthcare professional before starting any treatment or exercise program
. Since unconscious practices may worsen the symptoms, expert opinion should be sought.Frequently Asked Questions
1. Who is more likely to develop a cervical hernia?
Cervical hernia can occur in both young adults and the elderly. It is especially more common among those who work at a desk, lift heavy objects, or remain inactive for long periods.
2. What symptoms may indicate a cervical hernia?
Pain radiating to the neck, shoulders, or arms, numbness, tingling, loss of strength in the arms, decreased reflexes, and rarely dizziness may be signs of a cervical hernia.
3. What is the most effective diagnostic method?
Magnetic resonance imaging (MRI) is the most sensitive and detailed method for diagnosing cervical hernia.
4. Are exercises safe for every patient?
Not every exercise program is suitable for all patients. Individuals with a cervical hernia should follow programs recommended by a physician and prepared under the supervision of a physiotherapist.
5. Is massage beneficial for cervical hernia?
With appropriate techniques, it may help reduce muscle spasm and pain. However, massage may not be recommended in some cases; you should consult your doctor for suitability.
6. Can a cervical hernia heal on its own?
In mild and early-stage cases, complaints may subside with rest and exercise. In advanced cases with neurological symptoms, medical intervention may be required.
7. Is surgery mandatory?
Most cervical hernia patients can recover with non-surgical methods. Surgery is recommended only in certain advanced cases and when other methods fail.
8. Is long-term use of a neck collar harmful?
Yes, prolonged use may lead to muscle weakness. A neck collar should be used only for a short period and under medical supervision.
9. Does computer and phone use trigger cervical hernia?
Poor posture and prolonged improper positioning can strain the neck muscles and discs, increasing the risk of hernia.
10. Can cervical hernia recur?
Yes, especially if risk factors are not addressed and lifestyle is not changed, it may recur.
11. Which medications are used in the treatment of cervical hernia?
Painkillers, muscle relaxants, and anti-inflammatory drugs are generally prescribed. Medication should always be used under a doctor's supervision.
12. In which situations should you consult a doctor?
If you have complaints of pain, numbness, or loss of strength, or if your existing symptoms worsen, you should consult a healthcare professional without delay.
References
World Health Organization (WHO): “Musculoskeletal Conditions”
American Academy of Neurology (AAN): Cervical Radiculopathy Guidelines
European Spine Society (EuroSpine): Cervical Disc Herniation Recommendations
American Academy of Orthopaedic Surgeons (AAOS): Neck Pain and Cervical Disc Disease
Mayo Clinic: “Herniated Disk”
New England Journal of Medicine: “Cervical Radiculopathy”